
Conspiracy Archive
The Coronavirus Conspiracies
Claim: Face masks don't do anything
This is the claim that face masks don't do anything and are useless.



Well, let's just take a moment to think about that. This basic starting point I see people talking about usually starts from the conclusion, albeit subtextually, that the virus is an overblown flu or a hoax.
Let's take a step back for a moment. If we're to honestly seek the truth, let's put aside all conclusions and assumptions, review the evidence, and see where we land.
If the virus is just the flu or a hox, then you'd have a point, but you need to demonstrate that.Assuming that the virus is dangerous and exists (I have proven in the hoax page that it does exist), then it's perfectly rational to wear facemasks.
Using this as a starting point, let us look at the science regarding face masks.

From this Nature study called: "Respiratory virus shedding in exhaled breath and efficacy of face masks", they write:
"These viruses spread between humans through direct or indirect contact, respiratory droplets (including larger droplets that fall rapidly near the source as well as coarse aerosols with aerodynamic diameter >5 µm) and fine-particle aerosols (droplets and droplet nuclei with aerodynamic diameter ≤5 µm)"
So this gives us the baseline for understanding how virus' like Flu and Sars-Cov-2 spread. According to the introduction of this Science Daily study called: "Documentary Research of Human Respiratory Droplet Characteristics", they write:
"Patients produce droplets during breathing, speaking, coughing and sneezing. Pathogens attach to the droplets and transmit to the mouth, nasal and conjunctiva positions of susceptible populations within a close range and short time span. The susceptible population is infected and lead to the spread of the disease. Common droplet transmission diseases include the common cold, flu, tuberculosis, pathogen meningitis, etc."
By breathing, speaking, coughing and sneezing, you produce respiratory droplets that can infect others. It's vitally important to recognise you produce these whilst breathing and talking, not just coughing.
During the section on the mechanism of droplet formation they write:
"Epidemiology [8, 9] shows that most respiratory infections indoor are caused by droplet or microbial aerosol transmission. Among different size respiratory droplets, those of the large size deposit to the ground in 1 meter [10-13] or vaporize into droplet nuclei, the other of the relatively small suspend in the air for long time. These smaller droplets may carry more pathogens."
"According to documents, it is obtained that some health people make more droplets than others, the coughing droplet concentration is the largest, speaking second, breathing least."
When talking about droplet velocity and transmission, they write:
"The human mouth or nose can be assumed a spout, the expelled droplet velocity is important for predicting the transmission distances and trajectories[90-96,99-102]. The breathing droplet velocity is relatively small, and lower than coughing and sneezing. The ranges of breathing droplet velocity is 0.1 to 1m/s, the transmission distance is about 1m; the speaking droplet velocity is 2-10 m/s; the coughing droplet velocity reaches 10-20 m/s and it transmits more than 2m."
From the above, we can see that we produce potentially infections respiratory droplets by doing pretty much anything that involves us opening our mouths. Infectious droplets can exist in the air and infect other people.
OK, so what about masks? All I've done is shown that we have a massive capability to infect people without knowing about it.
Going back to the Nature study above
They studied virus shedding while using and not using a face mask. Viral shedding is basically when you shart shedding the virus. It's when you project the virus outside of yourself.
They write:
"We detected coronavirus in respiratory droplets and aerosols in 3 of 10 (30%) and 4 of 10 (40%) of the samples collected without face masks, respectively, but did not detect any virus in respiratory droplets or aerosols collected from participants wearing face masks, this difference was significant in aerosols and showed a trend toward reduced detection in respiratory droplets"
Here is the graph they provide showing the reduction in droplets with using face masks.

In the abstract, they write:
"Surgical face masks significantly reduced detection of influenza virus RNA in respiratory droplets and coronavirus RNA in aerosols, with a trend toward reduced detection of coronavirus RNA in respiratory droplets. Our results indicate that surgical face masks could prevent transmission of human coronaviruses and influenza viruses from symptomatic individuals."
OK, but what face masks? There are so many
That's true. For this, let's look at a study from the The Journal of Multidisciplinary Healthcare called "Transmission of communicable respiratory infections and facemasks."
They compared N95 face masks against face masks with ventilation at the back or sides of the facemask.
Here are two images that show the protection of masks without front-filtration, and normal N95 masks.


Their results say that:
"Experimental results showed that when droplets spread onto a person face-to-face over short distances, 92.3% to 99.5% of droplets were blocked by the front surface of the facemask, whereas only 0.5% to 7.7% of droplets reached the back of the facemask. Both facemasks A and B had near or over 99% protection efficiency, compared with that of 95.5% to 97% of surgical facemasks. Using the same filters as normal surgical masks, facemasks A and B provided more effective respiratory protection against communicable respiratory infections such as influenza and SARS by the location of the breathing pathway to the back of the facemasks."
Then, in the conclusion they write:
"Separating the breathing pathway from the virus-contaminated area in facemasks can provide more effective protection against communicable respiratory infections such as influenza and SARS."
The reason for this in the study is because they explain that virus' can still pass through masks if they're in a region you're breathing in. That's the basic summary of the findings.
But what about normal cloth masks?
In a study from the British Medical Journal Open called "A cluster randomised trial of cloth masks compared with medical masks in healthcare workers" published in 2015, they studied 1607 patients who used surgical masks, cloth masks, and a control group.
This study focused on Influenza-like illness (ILI). They write:
"An analysis by mask use showed ILI (RR=6.64, 95% CI 1.45 to 28.65) and laboratory-confirmed virus (RR=1.72, 95% CI 1.01 to 2.94) were significantly higher in the cloth masks group compared with the medical masks group. Penetration of cloth masks by particles was almost 97% and medical masks 44%."
"This study is the first RCT of cloth masks, and the results caution against the use of cloth masks. This is an important finding to inform occupational health and safety. Moisture retention, reuse of cloth masks and poor filtration may result in increased risk of infection. Further research is needed to inform the widespread use of cloth masks globally. However, as a precautionary measure, cloth masks should not be recommended for HCWs, particularly in high-risk situations, and guidelines need to be updated."
It's not all bad. On that same article, the authors address the cloth mask inadequacies in relation to the Covid-19 pandemic:
"We recommend that health workers should not work during the COVID-19 pandemic without respiratory protection as a matter of work health and safety. In addition, if health workers get infected, high rates of staff absenteeism from illness may also affect health system capacity to respond. Some health workers may still choose to work in inadequate PPE. In this case, the physical barrier provided by a cloth mask may afford some protection, but likely much less than a surgical mask or a respirator. "
"It is important to note that some subjects in the control arm wore surgical masks, which could explain why cloth masks performed poorly compared to the control group. We also did an analysis of all mask wearers, and the higher infection rate in cloth mask group persisted. The cloth masks may have been worse in our study because they were not washed well enough"
"If health workers choose to work using cloth masks, we suggest that they have at least two and cycle them so that each one can be washed and dried after daily use. Sanitizer spray or UV disinfection boxes can be used to clean them during breaks in a single day. These are pragmatic, rather than evidence-based suggestions, given the situation."
The missing piece of the puzzle
The two things you need to do to help stop the spread of the virus are:
-Not get infected
-Not to infect others
While cloth masks in a medical setting didn't fare well, this isn't related to healthy people's everyday use. When you cough, sneeze or even talk, you'll visibly see the droplets or spit you project outwards. Considering that these studies are dealing in measurements of µm (micrometres), that's important. 1 µm is 0.001 mm, it's so tiny you're not going to see it. The visible droplets and spit are much larger than this obviously. Wearing cotton masks will stop these droplets from moving past your mask. No mask, no stoppage.
But, also consider the two things above. Don't think so small where it's all about what you do and that's it. Think on the larger scale. If you wear a cotton mask, sure you're not stopping µm droplets entering your mask very efficiently, but what if everyone else is also wearing them? Taking a random number for example purposes, if cotton masks were 10% effective, if the person you're with is also wearing one then they've become 19% effective. It's not a definitive thing. The more people wear masks and socially distance, the more effective we are as a society. We exist in the broader context of our society, so thinking in terms of self isn't weighing up the situation properly.

There’s another point of interest when talking about masking and infection from COVID-19. Viral Inoculum is the amount of the virus you initially contract. You can either contract a small dose of the virus, a large dose, or anywhere in between. There’s also a term called viral load which is the amount of virus you have within your body - these aren’t the same thing.
In an article on the New England Journal of Medicine titled: Facial Masking for Covid-19 — Potential for “Variolation” as We Await a Vaccine.
Monica Gandhi, M.D., M.P.H., and George W. Rutherford, M.D write in this article about the utility of face masks in providing immunity. The hypothesis is that masks will stop a proportion of the virus from entering your body if you become infected. This as they explain, is thought to result in a lower viral inoculum, which in turn translates to a less severe, mild, or asymptomatic case of COVID-19. There is evidence elsewhere supporting this hypothesis and it looks like a strong conclusion.
“Recent virologic, epidemiologic, and ecologic data have led to the hypothesis that facial masking may also reduce the severity of disease among people who do become infected”
“This possibility is consistent with a long-standing theory of viral pathogenesis, which holds that the severity of disease is proportionate to the viral inoculum received.”
“With viral infections in which host immune responses play a predominant role in viral pathogenesis, such as SARS-CoV-2, high doses of viral inoculum can overwhelm and dysregulate innate immune defenses, increasing the severity of disease.”
“Since masks can filter out some virus-containing droplets (with filtering capacity determined by mask type),2 masking might reduce the inoculum that an exposed person inhales.”
“The typical rate of asymptomatic infection with SARS-CoV-2 was estimated to be 40% by the CDC in mid-July, but asymptomatic infection rates are reported to be higher than 80% in settings with universal facial masking, which provides observational evidence for this hypothesis.”
“we hypothesize that by reducing the viral inoculum, it would also increase the proportion of infected people who remain asymptomatic.”
So there are some extracts from the article these two doctors posted in the NEJM. Let’s take a look at the supporting evidence.
In a short communication (which is basically an article) from the Lancet Respiratory Medicine titled: Inoculum at the time of SARS-CoV-2 exposure and risk of disease severity
In this piece, they look at the hypothesis that viral inoculum plays a role in infection severity.
“Here, we report three clusters of individuals that were potentially exposed to distinct inoculum in Madrid. Overall each group developed divergent clinical forms of COVID-19. Our data support that a greater viral inoculum at the time of SARS-CoV-2 exposure might determine a higher risk of severe COVID-19.”
Now, while this idea looks pretty solid, the standard for what constitutes a theory or proof is very high. Despite it making perfect sense and having supporting evidence, the scientific community isn’t going to accept what makes sense, but instead what has been proven. See below:
“However, it remains unclear whether exposure to a greater viral inoculum could determine a higher risk for developing severe COVID-19. Although intuitive, it has been challenging to obtain such dose-response data.”
“We hypothesize that distinct sizes of viral inoculum at the time of exposure could explain their different illness course.”
Looking through this article, the sample size they used was extremely small. For this reason, I’m discounting this article, but the opening abstract is worth quoting, anyway. If we’re to get reliable data, it can’t be from clusters of 10 or 25 people.
In the Clinical Infectious Diseases journal from Oxford Academic is a study titled: Surgical Mask Partition Reduces the Risk of Noncontact Transmission in a Golden Syrian Hamster Model for Coronavirus Disease 2019 (COVID-19).
This one is quite interesting. They had 6 cages of hamsters in a confined space. They were separated into 2 groups of 3, separated by a fan blowing through a medical mask to simulate airborne transmission of viral particles. The walls around the cages offer some blockage, but all six cages share the same closed space.

They conducted three experiments. One where infected hamsters had their air fanned onto the non infected hamsters. A second where infected hamsters had their air fanned through a mask facing the away from the infected, blowing onto the non infected hamsters, and a third where the second experiment was reproduced with the mask flipped around.
The basic aim was to experiment with airborne transmission as a control standard, to simulate infectious individuals infecting others if they wore a mask, and the third to test the effect of wearing a mask against incoming infection.
To sum this up even more, the three experiments were airborne control, source control, and incoming infection prevention.
The experiment showed that the air strength was lower when the mask was placed in front of the fan. Notice in the graph shown, that the air velocity was lower with the mask covering the presumed wearer, than it was when switched around, showing that masks let in air easier than they let it out. I thought that was quite interesting.
While the sample size is low, and these are experiments on hamsters (which have been shown to have similar infection characteristics as us), it’s worth seeing what happened.
“In the first experiment, 6 of the 10 (60%) exposed naive hamsters sacrificed at 5 dpi (4 days after exposure) also developed similar clinical signs”
“In the second experiment in which the external surface of the mask was facing the naive hamsters, at 5 dpi (4 days after exposure), 2 of the 3 naive hamsters in each system (n = 8) were sacrificed. Only 1 out of 8 (12.5%) naive hamsters was SARS-CoV-2 RT-PCR-positive”
“In the third experiment, the external surface of the mask was facing the challenged index hamsters. At 5 dpi (4 days after exposure), 2 of the 3 naive hamsters in each system (n = 8) were sacrificed. Three out of 8 (37.5%) exposed naive hamsters developed clinical signs and were SARS-CoV-2 RT-PCR positive ”

What this shows (despite the small sample sizes) is that when a mask entered the equation, infection rates dropped regardless of whether they simulated the infected or the non-infested hamsters being masked.
Being masked reduced transmission by around half compared to no mask at all.

In the above graph you can see that viral load (the amount of virus present in the infected hamsters) after 7 days was consistently highest in the no mask scenario. The best outcomes were when they simulated the infected hamster wearing a mask.
It’s worth noting that the third experiment didn’t reach statistical significance. This could be in part to the small sample size (which is one of the problems with small sample sizes).
“In the infected naive hamsters, the nasal turbinate only showed mild degree of epithelial cell swelling and submucosal infiltration, whereas there were severe epithelial cell death, desquamation, and massive submucosal infiltration in the challenged control hamster”
Down in the discussion, the author sums up the findings.
“We showed that noncontact transmission occurred in 66.7% of unprotected naive hamsters after exposure to SARS-CoV-2-challenged hamsters for ≤96 hours. ”
“Moreover, the use of surgical mask partition to prevent emission of exhaled respiratory droplets from SARS-CoV-2-challenged index hamsters significantly reduced the transmission rate to 16.7% (P = .019). The use of surgical mask partition to protect naive hamsters reduced the transmission rate to 33.3%, although this did not reach statistical significance, likely because of the relatively small number of animals (P = .128). ”
“The intensity of exposure may affect the severity of viral infections as has been demonstrated in outbreaks of chickenpox, measles, and poliomyelitis [30–32]. The effect of virus inoculum on the severity of COVID-19 is evident when the histopathological changes and amount of viral N antigen expression in the respiratory tracts of the infected naive hamsters with or without protection by surgical mask partition was compared with those of the virus-challenged hamsters.”
“The protective effect of masking may not just determine the success or failure of SARS-CoV-2 transmission, but it may also determine the severity of COVID-19 in the case of successful transmission.“
“This report clearly showed that surgical masks could be partially effective in reducing the transmission of a well-known airborne pathogen Mycobacterium tuberculosis and corroborated with the results of the masking experiments in our hamster model of noncontact transmission of SARS-CoV-2.”
“Face mask usage may serve as source control by preventing dispersal of droplets during talking, sneezing, and coughing, and also reduce the risk of environmental contamination by SARS-CoV-2. Our results showed that masking of the challenged index appeared to be more important than masking the to-be-exposed healthy hamsters, which is consistent with the findings in a systematic review on influenza transmission”
An important note at the very end of the study when the limitations were discussed shows that one of the studies limitations might have even down-played the efficacy of masks.
“we could not determine if contact transmission has occurred among exposed naive hamsters housed in the same cage. This might have resulted in an underestimation of the protective efficacy of masks, which would otherwise be even more significant.”
I'm not someone who advocates the use of videos as proof of anything. We need research and evidence, and insight in order to make educated decisions about what is and isn't likely, or even correct.
However, Monica Gandhi is a big source of information online about viral inoculum reducing severity of infection. She has been on many websites I've found, and most notably, she was on the ZdogMD YouTube channel discussing masks. I will link the full video as it was fascinating to me to watch.

Summarising everything, we can see that we expel infectious droplets by breathing, speaking, coughing and sneezing. Masks with back or side ventilation help protect against infection as the breathable area isn't exposed to the virus as much. N95 masks are helpful but not complete protection. Cloth masks don't provide much protection according to the BMJ study, but the author acknowledges the control group used N95 masks and the cloth masks might not have been properly cared for.
So for the average person, cloth masks are better than nothing and may provide some measure of protection if you have multiple masks, clean them after use, and disinfect them.
Furthermore, there is a good reason to believe that the hypothesis that masks, although not able to block incoming viral infections, might work to reduce your viral inoculum which could result in milder or asymptomatic infections. It doesn't have a huge amount of supporting evidence which is why it's a hypothesis, but there is a good amount of supporting information out there.
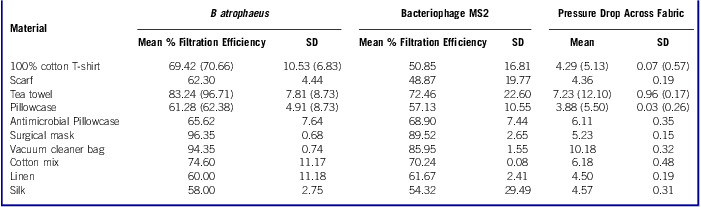
Additionally, there is a study out of Cambridge called Testing the Efficacy of Homemade Masks: Would They Protect in an Influenza Pandemic?. In this study from 2013 they tested different types of homemade masks and used surgical masks as a control. The testing part we're interested in is the virus testing. Now just a reminder, this was from 2013 and doesn't test the coronavirus. The subject of their testing:
"Bacteriophage MS2 (MCIMB10108) is a nonenveloped single-stranded RNA coliphage, 23 nm in diameter, known to survive the stresses of aerosolization."
The following tangent is a snippet from a page called the Faculty of Pharmaceutical Medicine. This isn't a study and is authored by a single doctor albeit with input from five other doctors. Keep that in mind before using this as a gospel reference. I mention this just to get a sense of the size of the COVID-19 particle itself. The page reviews the current pandemic and says:
"Human coronavirus particles are generally spherical, 120-160nm diameter and typically decorated with large (~20 nm), club- or petal-shaped surface projections"
I bring this up just to put into context somewhat the Cambridge study above. The virus sample they used in the study was comparable to human coronavirus. I might be wrong on this comparison, though. So back to the Cambridge study. They write in their results summary:
"The median-fit factor of the homemade masks was one-half that of the surgical masks. Both masks significantly reduced the number of microorganisms expelled by volunteers, although the surgical mask was 3 times more effective in blocking transmission than the homemade mask."
Finishing up in their conclusion:
"Our findings suggest that a homemade mask should only be considered as a last resort to prevent droplet transmission from infected individuals, but it would be better than no protection."
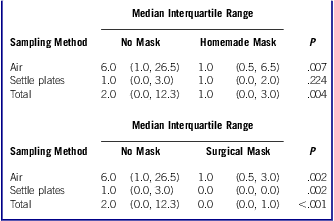
Just for the sake of clarity, when they write interquartile range this is what they're referring to in statistical analysis:


I've been looking at some interesting information after writing this page originally. Here is a paper in MIT from the Journal of Fluid Mechanics titled Violent expiratory events: on coughing and sneezing. This paper describes the way that coughing and sneezing produce gas clouds and spread airborne pathogens.
"Our combined experimental and theoretical study has shown how particles can be suspended in turbulent clouds, their range thus being extended."
"The turbulent multiphase cloud plays a critical role in extending the range of the majority of pathogen-bearing drops that accompany human coughs and sneezes. Smaller droplets (less than 50μm diameter) can remain suspended in the cloud long enough for the cough to reach heights where ventilation systems can be contaminated (4–6 m). A droplet of diameterd=10μm evaporates in0.027 s, during which it would fall a distance of approximately 0.08 mm at a settling speed of approximately 3 mm s−1. It would thus clearly remain suspended in a cough or sneeze cloud metres away from the cougher. Indeed, the cloud model presented in this study predicts that the range of droplets of diameterd6100μm would be extended by a factor of 5 to more than 200"
"The ambient conditions also influence the buoyancy of the cloud and so the range of contamination of its suspended droplets."
From this Nature article about this study:
"thanks to the cloud dynamics, many of the larger droplets can travel up to 8 metres for a sneeze and 6 metres for a cough, depending on the environmental conditions, and stay suspended for up to 10 minutes — far enough and long enough to reach someone at the other end of a large room, not to mention the ceiling ventilation system."
This shows the important of wearing a mask - particuarly inside. In an indoors setting, then your coughs and sneezes can stay boiuyant in the air, travel quite a distance and go pretty high. Without airflow which is present outside or in a room that's well ventilated, the conditions allow these clouds to thay bouyant.

What you see here is a human cough photographed and calculated from the New England Journal of Medicine. The air currents (which can carry viral particles) can be seen through a clever photography method.
If you want to see the video here's a link. It's a little hard to get working as the player is unnecessarily tiny.
In the Canadian Journal of Ophthalmology in a paper titled Utility of patient face masks to limit droplet spread from simulated coughs at the slit lamp, they experimented with different types of masks and measured droplets in and out of the mask with fluorescent dye after simulated coughes.
"In the simulation involving the improperly positioned surgical mask, droplets were identified on the shoulders, arms, and gloves of the examiner as well as the slit lamp, floor, and walls. With the surgical mask properly positioned, the examiner was clear of droplets; however, some droplets were noted on the side bars close to the chin rest of the slit lamp. No droplets were identified on the examiner or the slit lamp in the repeat simulation with the use of the N95 mask. A view of the inside of the mask also revealed that droplets were contained within the mask."
It's the same thing again. N95 masks are really effective. Cloth masks are less so but they do help; they do something. Having the mask under your nose resulted in a clear increase in spread particles. If you wear a mask like this, you're not really doing anything.
"Our findings suggest that the use of a properly fitted mask on the patient as an adjunct to the current standard PPE used by the examiner, and the breath shield is essential for limiting droplet dissemination during slit-lamp examinations."
"These findings are consistent with other studies that have demonstrated reduced droplet transmission when wearing a face mask."
"Overall, this simulation demonstrates the potential spread of droplets during a slit-lamp examination from a patient cough onto the examiner, equipment, and room. Based on this, our recommendations for the use of masks for patients include the following: (i) patients should wear a mask during slit-lamp examinations (including a well-fitted cloth mask if it is the only available option); (ii) correct positioning of the mask is critical, and an improperly fitted mask may provide a false reassurance of protection"
The Royal Society of Publishing has a study titled A schlieren optical study of the human cough with and without wearing masks for aerosol infection control which used this very method above in context of an N95 and surgical mask.
"They first show an unmasked cough (figure 5a), which produces a turbulent jet (directed downwards at about a 30° angle in this case) extending across the schlieren field-of-view towards the second volunteer. The effect of the surgical mask is to block the forward motion of the cough jet (figure 5b) and to redirect it upwards and downwards owing to leakage around the relatively loose fit of the mask. The tighter seal of the N95 mask to the volunteer's face prevents some of this leakage (figure 5c) forcing more of the cough through the front of the mask at a relatively low airspeed. The resulting cough effluent is then transported upwards and away from the second volunteer by the thermal plume of the coughing volunteer."


The left shows the paragraph above, while the right image shows the air distribution of a cough wearing an N95 and surgical mask.
"Unmasked coughing produces a turbulent air jet extending across the present schlieren field-of-view and probably well beyond it. As already described, this jet may contain infectious aerosolized particles or droplets."
On surgical masks:
"Wearing a standard surgical mask effectively blocks the forward momentum of the cough jet and its aerosol content, although the loose fit of the mask allows much of the air ejected by the cough to leak around the top, bottom and especially the sides of the mask. This leakage air also has minimal momentum, but is usually entrained into the thermal plume of the cougher rather than being projected in such a way as to affect others"
On N95 masks:
"Wearing an N95 mask reduces the leakage around the edges of the mask during coughing, because of its tighter seal to the facial skin (especially with formal fit-testing). However, this improved seal increases the pressure inside the mask when the volunteer coughs, thereby forcing more of the air ejected by the cough directly through the front of the N95 mask while decelerating it significantly"
"Even so, both surgical and N95 masks serve an important purpose in preventing airborne virus transmission: they prevent the expelled particle-containing air of a cough from being projected forward as a rapid turbulent jet over distances sufficient to reach the breathing zones of other individuals."
Something very important at the bottom of the study:
"Previous studies on surgical and N95 masks have found that their efficiency at removing aerosol particles depends upon several factors, including the velocity of the airflow passing through the mask, the degree of leakage around the mask, and the particle size distribution to be filtered"
"However, all these studies investigated the mask's efficiency in protecting the wearer from environmental airborne hazards, rather than the reverse problem of containment efficiency when the wearer is the potential source of infectious aerosols."
Finally, while many of these studies focus on virus transmission and respiratory droplets, study from Frontiers in Medicine titled Textile Masks and Surface Covers—A Spray Simulation Method and a “Universal Droplet Reduction Model” Against Respiratory Pandemics that explored macro-droplet suppression from home-made masks:
"all textiles, tested as ‘single-layers’, significantly and reproducibly (between institutions) reduced the ejection of macro-droplets, and the traffic of micro-droplets to <25.5-34cm (linear regression adj.-P<0.001, compared to 180cm with no textile barrier"
"Remarkably, spray experiments with ‘two-layers’ (of 100%-combed cotton, common in t-shirts; and 100% polyester, in sports jerseys) completely prevented the ejection of large macro-droplets (100% EnDC prevention), and drastically reduced the ejection of micro-droplets by a factor of 5.16 Log2, which is equivalent to a 97.2% droplet reduction"
"Together, experiments indicate that two-layers of household textiles are as effective as medical masks preventing EnDC(environmental droplet contamination), and that more breathable materials in ≥2-layers could be effectively used if individuals deem two-layer, ‘denser’ textiles too air-restrictive. "
From the European Respiratory Journal in an article titled: Universal use of face masks for success against COVID-19: evidence and implications for prevention policies, they write:
"we strongly support the use of cloth masks as a simple, economic and sustainable alternative to surgical masks as a means of source control for general community use, so that disposable surgical masks and N95 respirators can be reserved for use in healthcare facilities. Such an intervention is likely to be life saving in many resource-limited settings."
In a study titled Visualizing the effectiveness of face masks in obstructing respiratory jets from the API Journal the Phsysics of Fluid:
"These masks were able to curtail the speed and range of the respiratory jets significantly, albeit with some leakage through the mask material and from small gaps along the edges. Importantly, uncovered emulated coughs were able to travel notably farther than the currently recommended 6-ft distancing guideline."
"The larger droplets (diameter >100 µm) are observed to follow ballistic trajectories under the effects of gravity and aerodynamic drag.20,31 Intermediate-sized droplets20,31,32 may get carried over considerable distances within a multiphase turbulent cloud.33–35 The smallest droplets and particles (diameter < 5 µm–10 µm) may remain suspended in the air indefinitely, until they are carried away by a light breeze or ventilation airflow.20,32"
"After being expelled into the ambient environment, the respiratory droplets experience varying degrees of evaporation depending on their size, ambient humidity, and temperature. The smallest droplets may undergo complete evaporation, leaving behind a dried-out spherical mass consisting of the particulate contents (e.g., pathogens), which are referred to as “droplet nuclei.”"
"Nonetheless, the evidence suggests that masks and other face coverings are effective in stopping larger droplets, which, although fewer in number compared to the smaller droplets and nuclei, constitute a large fraction of the total volume of the ejected respiratory fluid."
"We observe that the mask is able to arrest the forward motion of the tracer droplets almost completely. There is minimal forward leakage through the material, and most of the tracer-escape happens from the gap between the nose and the mask along the top edge."
"We observe that a single-layer bandana-style covering can reduce the range of the expelled jet to some extent, compared to an uncovered cough. Importantly, both the material and construction techniques have a notable impact on the masks’ stopping-capability. The stitched mask made of quilting cotton was observed to be the most effective, followed by the commercial mask, the folded handkerchief, and, finally, the bandana."
"Additionally, the masks may get saturated after prolonged use, which might also influence their filtration capability. We reiterate that although the non-medical masks tested in this study experienced varying degrees of flow leakage, they are likely to be effective in stopping larger respiratory droplets."
"Promoting widespread awareness of effective preventative measures is crucial, given the high likelihood of a resurgence of COVID-19 infections in the fall and winter."
Here are some images from their study.



For those who like videos:
Even more studies
In a randomised study from the National Institute of Health from Feb 2009 titled Face Mask Use and Control of Respiratory Virus Transmission in Households, they randomised roughly 150 families with atleast one child under 16 who was sick to wear 2 types of mask, and a control arm wearing no mask. They measured mask adherance and infection over time.
"adherent use of P2 or surgical masks significantly reduces the risk for ILI infection, with a hazard ratio equal to 0.26"
"Under the less likely assumption that the incubation period is equal to 2 days, the quantified effect of complying with P2 or surgical mask use remains strong, although borderline significant"
"Although our study suggests that community use of face masks is unlikely to be an effective control policy for seasonal respiratory diseases, adherent mask users had a significant reduction in the risk for clinical infection."
"Therefore, although we found that distributing masks during seasonal winter influenza outbreaks is an ineffective control measure characterized by low adherence, results indicate the potential efficacy of masks in contexts where a larger adherence may be expected, such as during a severe influenza pandemic or other emerging infection."
Or in other words: Masks are effective if most people use them. This is precisely why you wearing a mask is important. It's not enough for the person who doesn't want to be infected to wear a mask - the problem is larger than that.
"We estimated that, irrespective of the assumed value for the incubation period (1 or 2 days), the relative reduction in the daily risk of acquiring a respiratory infection associated with adherent mask use (P2 or surgical) was in the range of 60%–80%."
"The causal link cannot be demonstrated because adherence was not randomized in the trial. Although we found no significant difference in handwashing practices between adherent and non-adherent mask users, it is possible that adherent mask use is correlated with other, unobserved variables that reduce the risk of infection."
This is why we need more than one study. The body of evidence showing the efficacy of face masks is growing in 2020 especially.
"For new or emerging respiratory virus infections, no pharmaceutical interventions may be available. Even with seasonal influenza, widespread oseltamivir resistance in influenza virus A (H1N1) strains have recently been reported (32). Masks may therefore play an important role in reducing transmission."
In this study regarding health workers and mask usage from Infectious Disease Modelling titled To mask or not to mask: Modeling the potential for face mask use by the general public to curtail the COVID-19 pandemic:
"Randomised controlled trials in health care workers showed that respirators, if worn continually during a shift, were effective but not if worn intermittently. Medical masks were not effective, and cloth masks even less effective."
Note that this is in context of health workers where they are directly caring for many sick patients coughing and sneezing all day. This setting is drastically different then a general public usage situation.
"The study suggests that community mask use by well people could be beneficial, particularly for COVID-19, where transmission may be pre-symptomatic. The studies of masks as source control also suggest a benefit, and may be important during the COVID-19 pandemic in universal community face mask use as well as in health care settings. Trials in healthcare workers support the use of respirators continuously during a shift. This may prevent health worker infections and deaths from COVID-19, as aerosolisation in the hospital setting has been documented."

Her'e's a study out of Travel Medicine and Infectious Disease titled: Efficacy of face mask in preventing respiratory virus transmission: A systematic review and meta-analysis.
They went through and included studies based on several quality control criteria which filtered down to 21 studies on protection from wearing a mask.
"The 21 studies, involving 8,686 participants, showed that masks were generally effective in preventing the spread of respiratory viruses. After wearing a mask, the risk of contracting RVIs was significantly reduced"
"For non-HCWs, similar protective effects were also observed in Asian (OR = 0.51, 95% CI = 0.34–0.78, I2 = 45%) and Western countries (OR = 0.46, 95% CI = 0.34–0.63, I2 = 57%)."
"In the subgroups based on different study designs, protective effects of wearing mask were significant in cluster randomized trials (OR = 0.65, 95% CI = 0.47–0.91, I2 = 20%) and observational studies (OR = 0.24, 95% CI = 0.15–0.38, I2 = 54%)"
"This meta-analysis of the 21 studies provided the latest state-of-art evidence on the efficacy of masks in preventing the transmission of RVIs. Our data show that the protective effects of masks against RVIs were not only significant for both HCWs and non-HCWs, but also consistent between Asian and Western populations."
"According to our analysis, wearing masks significantly reduced the risk of infection among HCWs by 80%. It is noteworthy that, none of the 278 HCWs wearing N95 masks in quarantined areas were infected by SARS-CoV-2 yet, 10 of the 215 HCWs who did not wear masks in the open areas were infected"
"Accumulative data showed that people with older age, immunosuppressed state and systematic commodities are at higher risk for severe COVID-19 infection [[45], [46], [47]], and therefore, should be protected with proper measures (e.g. prophylactic masking) during the current pandemic. In addition, those who have close contact with those populations at high risks of contracting RVIs should consider wearing masks as well."
"More importantly, our data showed that masks worn by non-HCWs can also effectively prevent the spread of respiratory viruses and reduce the risk of virus infection by 56% in non-household settings, indicating the potential benefits of wearing masks for the general public. Moreover, significant protective effects were found in the study conducted in the general population [17], indicating the potential benefits of wearing masks for the general public."
"Two household studies included in our analysis reported low facemask adherence among household contacts [23,24], which might explain the poor protective effects from these studies. In contrast, Suess et al. reported a good compliance, which showed a significant protective effect [29]. These findings implicated that proper use of masks has an impact on the effectiveness of preventing RVIs"
"The risk of influenza, SARS, and COVID-19 infection were reduced by 45%, 74%, and 96% by wearing masks, respectively, which were consistent with previous meta-analyses during the SARS outbreaks [9,53]."
"This would suggest that the proper use of masks might play a significant role in public health efforts to suppress the spread of RVIs, regardless of the geographic locations, especially during an outbreak."

I rate this false. Cloth masks aren't perfect, but they're better than nothing and emerging information is showing that they can have great utility, especially in the potential to reduce viral inoculum reducing the severity of infection. They can prevent you from ejecting droplets that can infect others. Something providing less than total protection doesn't mean having no protection is better.
Also, consider the protection if not only you but everyone else wears a mask. It may help protect the overall community. You could also (if the viral inoculum hypothesis is accurate) be achieving herd immunity easier by having a reduced case of COVID-19 because you wore a mask.
Again, some protection is better than no protection, and emerging evidence is further supporting the utility of both proection, and there is a substantial body of evidence showing the efficacy of masks preventing spread. Advocates for no masks I see always ignore this and think only in terms of themselves and in black and white terms such as "cloth can't stop a virus". The argument against facemasks I have seen revolve around giving you a false sense of safety and encouraging you to be complacent and as such, less careful.
Can't we keep our sense of safety and caution while providing as much protection for ourselves and others that we can? I'm not convinced of the argument against them whatsoever. The arguments I've heard on every claim has been unfounded.
The science seems pretty uniform on the utility of face masks for preventing spread which is called source control, and there is a good body of information showing there may be serious utility in masks offering proection by lowering viral inoculum. The nuance here being that studies I've seen saying masks don't prevent inward infection, don't look at infection severity.
I originally marked this claim very misleading, but after more digging and reading more studies, this is outright false.

